Table of Contents
While it may seem counterintuitive, exercise for POTS management and physical conditioning habits can play a powerful role in improving symptoms of POTS. Postural Orthostatic Tachycardia Syndrome (POTS) is a form of dysautonomia that affects circulation (blood flow). Building tolerance to activity through a carefully structured program helps patients regain function and reduce episodes of orthostatic intolerance.
Currently, we view these programs not just as “working out,” but as neuro-rehabilitation. When appropriately designed, a physical conditioning program doesn’t just help with strength and stamina; it literally “re-trains” the autonomic nervous system. By strengthening the communication between the brain and the blood vessels, exercise improves venous return and helps stabilize blood pressure and heart rate, essentially teaching the body how to handle gravity again.
Why Exercise is Challenging for People with POTS
For individuals with POTS, especially in the early stages of diagnosis or during symptom flares, physical activity can feel like an impossible hurdle. Simple actions like standing or walking can trigger a rapid heartbeat, dizziness, fatigue, or even fainting.

Currently, specialists recognize that this challenge is rooted in Gravity Intolerance. When a person with POTS stands, blood tends to pool in the lower extremities and the abdomen. Because the autonomic nervous system doesn’t effectively “squeeze” the veins to push that blood back up, the heart has to work overtime to keep the brain oxygenated. This creates a state of Cerebral Hypoperfusion—where the brain isn’t getting quite enough blood—leading to the hallmark dizziness and “brain fog” that makes traditional upright exercise feel like a threat to the system rather than a benefit.
However, when approached with caution and patience, movement can be transformed from a symptom trigger into a powerful tool for recovery. The secret lies in removing the “gravity tax” by starting in horizontal or seated positions.
Evidence-Based Benefits of Exercise for POTS Patients
Numerous studies show that graded physical conditioning is one of the most effective non-pharmacological treatments for POTS. Established protocols, such as the Levine Protocol (Vanderbilt) and the CHOP Protocol (Children’s Hospital of Philadelphia), have proven that slowly increasing cardiovascular activity—specifically starting in recumbent or horizontal positions—can recalibrate the heart’s response to gravity.

Modern clinical research highlights these specific benefits:
- Cardiac Remodeling & Stroke Volume: Consistent exercise can actually increase the heart’s left ventricular mass and chamber size. This allows the heart to pump more blood with less effort (higher stroke volume), which naturally lowers the heart rate.
- Expansion of Total Blood Volume: Physical conditioning naturally signals the body to expand its plasma and red blood cell volume, providing a vital “buffer” against the hypovolemia often seen in POTS.
- Enhanced Autonomic Stability: Graded exercise improves vagal tone (the “rest and digest” signal), helping to dampen the overactive sympathetic “fight or flight” response that causes palpitations and anxiety.
- The “Muscle Pump” Effect: Strengthening the skeletal muscles in the legs and core provides a mechanical “squeeze” on the veins, assisting the heart by forcing pooled blood back up to the brain.
- Improved Cerebral Perfusion: Better circulation leads to more consistent blood flow to the brain, which is the primary driver in reducing the “brain fog” and cognitive fatigue patients report.
Key Principles for Exercise and Physical Conditioning

The cornerstone of safe and effective exercise with POTS is a gradual, consistent approach. Modern clinical guidance emphasizes these four pillars:
1. Start Slow and Low (Recumbent First)
Until your body can handle the “gravity tax,” keep your head and heart on the same horizontal plane. Use recumbent exercises like rowing machines, swimming, or stationary bikes with a backrest. These positions reduce blood pooling in the legs and abdomen, allowing you to strengthen your heart without triggering a massive spike in heart rate.
2. Prioritize the “Muscle Pump” (Lower Body & Core)
Current protocols now emphasize resistance training early in the process. Building muscle in the calves, thighs, and glutes creates a mechanical “squeeze” on your veins. This “second heart” helps push blood back up to the chest. Similarly, a strong core acts like built-in compression, preventing blood from pooling in the abdominal area.
3. Frequency and HRV Over Intensity
Consistency is more important than “pushing through.” Start with short sessions (5–10 minutes) several times per week.
- The HRV Factor: Many patients now use Heart Rate Variability (HRV) to guide their daily intensity. If your HRV is low (indicating a stressed autonomic nervous system), it is often better to stick to light stretching or floor-based yoga rather than a full cardio session to avoid a “crash.”
4. The “Volume Load” (Hydrate and Salt)
Exercise naturally causes fluid loss through sweat, which can be disastrous for a POTS patient. Ensure you “pre-load” with 16–20 oz of a high-osmolality electrolyte drink and extra sodium 30 minutes before activity. This expands your blood volume, making the heart’s job significantly easier during the workout.

5. Monitor and Adjust
Use a heart rate monitor to stay within your prescribed zones. While the Karvonen formula is a great starting point for calculating a POTS-adjusted max heart rate, remember that your “safe zone” may shift depending on the temperature, your sleep quality, and where you are in your recovery journey.
Recommended Exercise Routine for POTS Patients
Here is a general progression that can be customized based on individual tolerance and physician guidance.
Phase 1: Recumbent Training (Weeks 1–4)
Stretching or yoga on the floor
Recumbent bike: 5–10 minutes
Rowing machine: 3–5 minutes
Swimming or water aerobics

Phase 2: Transitional Training (Weeks 5–8)
- Increase recumbent cardio to 20–30 minutes
- Begin upright exercises slowly (marching in place, walking indoors)
- Add light resistance training (resistance bands, body weight)
Phase 3: Upright Conditioning (Weeks 9+)
Standing yoga or tai chi
Elliptical machine
Strength training with light weights
Common Challenges and How to Overcome Them
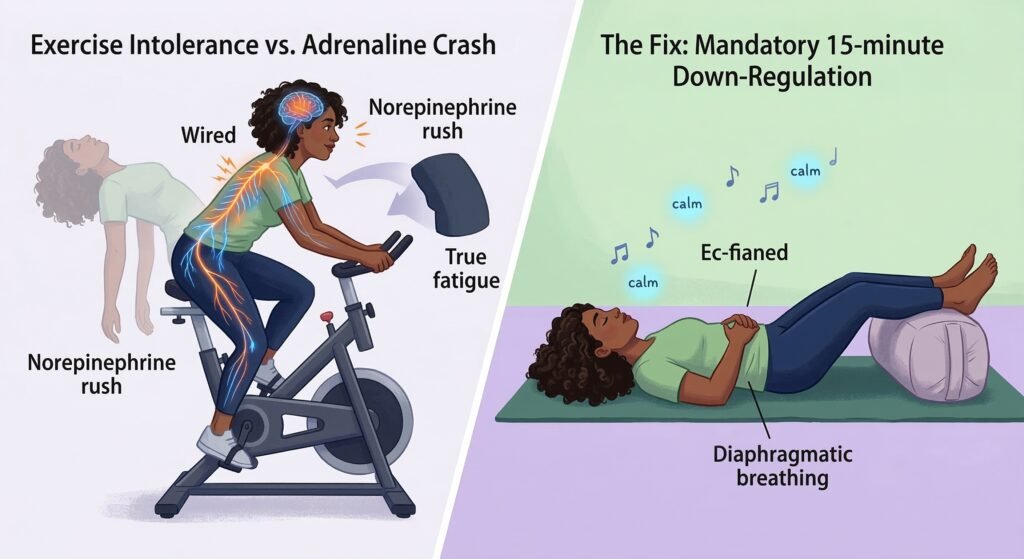
1. Exercise Intolerance vs. The “Adrenaline Crash”
Many patients—particularly those with a hyperadrenergic component—feel surprisingly “fine” or even “wired” during a workout, only to collapse an hour later. This is often an adrenaline dump (norepinephrine) masking the body’s fatigue.
- The Fix: Implement a mandatory 15-minute “Down-Regulation” cool-down. This involves lying flat with your legs elevated, practicing diaphragmatic (belly) breathing, and listening to calming music. This signals your nervous system to switch from “fight-or-flight” back to “rest-and-digest” before you stop moving.
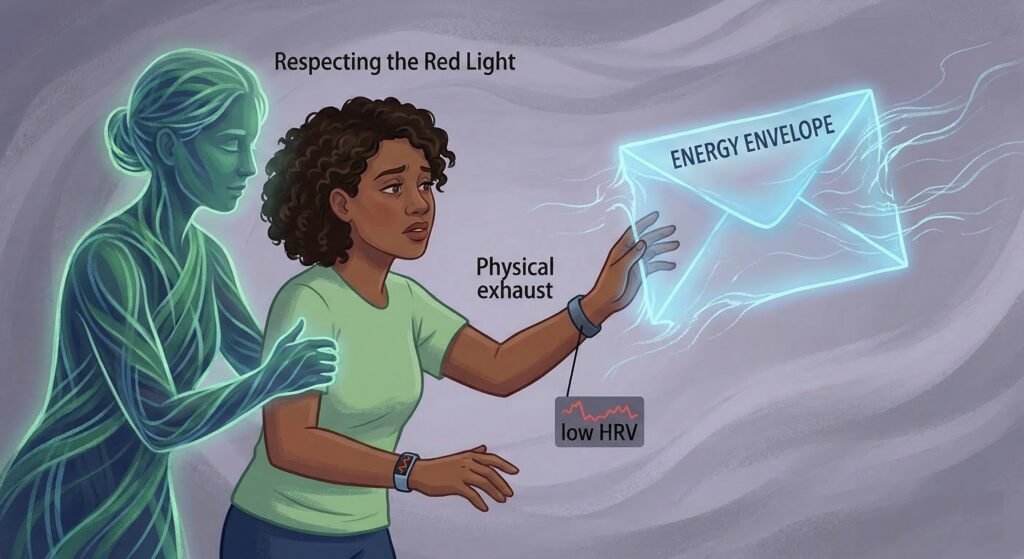
2. Managing Fatigue and PEM (The “Energy Envelope”)
If you have overlapping ME/CFS or Long COVID, the “push-pull” of exercise can be dangerous. Post-Exertional Malaise (PEM) is a distinct worsening of symptoms that occurs 12–48 hours after activity.
The Fix: Use Heart Rate Variability (HRV) Pacing. If your wearable device shows a low HRV (high stress) in the morning, your “energy envelope” for that day is small. On these days, skip the cardio and do 5 minutes of floor stretching instead. Respecting your “red light” days prevents the multi-day crashes that derail progress.
3. Overcoming “Kinesiophobia” (Fear of Movement)
When movement has caused pain or fainting in the past, your brain naturally develops a fear of exercise. This is a survival mechanism, but it can lead to further deconditioning.
The Fix: Use the “Floor-First” Strategy. Tell your brain it’s safe by staying on the ground. Doing leg lifts, glute bridges, or seated resistance band work eliminates the fear of fainting (since you’re already down), allowing you to build strength without the psychological stress of orthostatic triggers.
4. Mental Barriers and “Medical Gaslighting”
Dealing with a chronic, invisible illness is mentally exhausting. Many patients have been told their symptoms are “just anxiety,” which makes it hard to trust a new exercise plan.
The Fix: Track Micro-Wins. Don’t track “miles” or “calories.” Track “minutes upright” or “reps completed without a heart rate spike.” Seeing these objective data points in a journal helps counteract the mental toll of the illness and proves to your brain that progress is happening, even if it’s slow.
Combining Exercise with Other Lifestyle Strategies
Integrating exercise with other lifestyle habits creates a “synergy” that boosts overall improvement. Think of these strategies as the foundation that allows your physical conditioning to actually take hold.
Medical-Grade Compression (The “External Squeeze”)
Exercise causes blood vessels to naturally dilate (widen) to shed heat. In POTS, this can lead to massive blood pooling.
- The Strategy: Wear waist-high compression (20-30 mmHg) or an abdominal binder during your workouts. Modern research confirms that compressing the abdomen and “splanchnic bed” (the large blood reservoir in your gut) is far more effective at improving exercise tolerance than knee-high socks alone.
The Anti-Inflammatory “Fuel” Plan
A body in a state of chronic inflammation is less likely to recover well from the stress of exercise.
- The Strategy: Focus on a nutrient-dense, anti-inflammatory diet. This helps reduce “flares” that can sideline your progress for weeks. Many patients find that reducing high-histamine foods or processed sugars helps stabilize the “jittery” feeling often mistaken for exercise-induced anxiety.

Structured Sleep Hygiene & Circadian Rhythm
The autonomic nervous system does its most important “repairs” during deep sleep. If you are sleep-deprived, your resting heart rate will be higher, and your exercise tolerance will drop significantly.
- The Strategy: Maintain a consistent sleep-wake cycle. In the morning, get natural sunlight in your eyes as soon as possible to help regulate your cortisol and melatonin cycles, which are often dysregulated in dysautonomia.
Diaphragmatic Breathing (Vagal Tone Training)
If your heart rate stays high long after you’ve finished exercising, your “braking system” (the parasympathetic nervous system) needs help.
- The Strategy: Integrate 5–10 minutes of diaphragmatic (belly) breathing immediately following a workout. By stimulating the vagus nerve, you can manually “tell” your heart to slow down and move your body into a recovery state.
Temperature Regulation (The Cooling Strategy)
Heat is a potent vasodilator and a major trigger for POTS symptoms during exercise.
- The Strategy: Exercise in a cool environment, use a fan, or wear a cooling vest. Keeping your core temperature stable prevents the “fluid dump” that happens when your body tries to cool itself down via surface-level blood flow.
When to Seek Professional Support
While self-guided programs like the Levine or CHOP protocols are excellent starting points, consulting a professional can help you navigate the “plateaus” and “crashes” that often stall progress.
Seeking a POTS-Literate Physical Therapist
Not all physical therapists are trained in autonomic dysfunction. A specialist will look beyond just muscle strength; they will evaluate your orthostatic vitals during movement and help you find your specific “anaerobic threshold.” This ensures you are training in a zone that builds your heart without overtaxing your nervous system.
Specialized Autonomic Clinics and Cardiac Rehab
For those with severe symptoms or complex comorbidities (like hEDS or MCAS), supervised exercise in a cardiac rehab setting can be a lifesaver. These programs provide:
- Continuous ECG monitoring to see exactly what your heart is doing in real-time.
- Immediate intervention if your blood pressure or heart rate becomes unstable.
- Medical-grade equipment like specialized recumbent rowers or NuSteps that are often unavailable in standard gyms.
The Role of an Exercise Physiologist
If you are transitioning from recumbent to upright exercise, an exercise physiologist can help you design a Transitional Training Plan. They focus on the science of how your muscles use oxygen and can provide a data-driven roadmap to help you eventually stand and walk with confidence.
When Your Symptoms “Pivot”
If you find that your usual routine is suddenly causing new symptoms—such as extreme “adrenaline dumps,” prolonged insomnia, or joint pain—it is time to seek professional support. These “pivots” often indicate that your baseline has shifted and your protocol needs a professional adjustment.

GnarlyTree | PERSONAL STORIES WITH POTS
My Indoor Garden for Juicing | Easy Growing
A simple guide to growing fresh greens indoors for juicing, hydration support, and nutrient‑rich daily habits.
FAQ: Exercise and POTS Management
1. Can people with POTS really benefit from exercise? Yes. When done gradually and safely, exercise is one of the most effective ways to “re-train” the autonomic nervous system. It improves blood volume, increases the heart’s pumping efficiency, and helps regulate heart rate, leading to better overall symptom control.
2. Why is traditional exercise so difficult for people with POTS? It comes down to “gravity tax.” Upright activity (like running or standing weights) causes blood to pool in the lower body. This starves the brain of oxygen and forces the heart to race to compensate. Currently, we bypass this by starting with horizontal or seated movements.
3. What kind of exercise is safest to start with? Recumbent exercises are the gold standard. Rowing, recumbent biking, and swimming are safest because they keep your head and heart on a level plane, which reduces blood pooling and minimizes the risk of dizziness or fainting.
4. How should I structure my exercise routine? Success follows a “Slow and Low” progression. Start with short, low-intensity sessions (5–10 minutes) and focus on increasing your duration (how long you go) before you ever increase your intensity (how hard you go).
5. Should I track my heart rate during workouts? Absolutely. Monitoring heart rate helps you stay within a “safe zone” where you are strengthening your heart without triggering an adrenaline crash. Many patients currently use the Karvonen formula for a POTS-adjusted target, but using Heart Rate Variability (HRV) to check your recovery status each morning is an even more advanced way to avoid overtraining.
6. How do hydration and salt affect my workout? They are your “fuel.” Increasing sodium and fluids before exercise expands your blood volume, which makes it easier for your heart to pump while you move. Without this “volume loading,” exercise can feel significantly more taxing and may lead to a post-workout flare.
7. What if my symptoms worsen after working out? This is a sign to pivot, not quit. Dial back the duration or intensity of your next session. If you experience a “crash” that lasts more than 24 hours, it’s a signal that your nervous system was overtaxed. Focus on recumbent strength training and very slow cool-downs until your baseline stabilizes.
8. Is it okay to exercise with overlapping conditions like ME/CFS? Yes, but the rules change. For those with Post-Exertional Malaise (PEM), traditional “pushing” is dangerous. You must use Pacing Strategies and “Energy Envelopes,” prioritizing rest and very short bursts of movement that do not push your heart rate into a high-stress zone.
9. how can I stay motivated when I feel so sick? Shift your definition of “winning.” Don’t compare yourself to healthy athletes. Track micro-goals—like completing 5 minutes of floor exercises or hitting your hydration targets. Joining online communities of fellow “POTSies” can provide the peer support needed to stay consistent on the hard days.
10. When should I seek professional help? If you feel stuck, keep “crashing,” or have complex comorbidities like hEDS, seek out a POTS-literate physical therapist or an autonomic specialist. They can provide the medical supervision and data-driven adjustments needed to ensure your progress is safe and sustainable.
Conclusion: Building Strength, Stability, and Confidence
Exercise for POTS management and physical conditioning habits are a vital part of reclaiming your life from dysautonomia. While the road to building tolerance may be slow and filled with plateaus, it is often incredibly rewarding.
A carefully designed routine—focused on recumbent cardio, lower-body strength, and autonomic regulation—improves cardiovascular health, enhances quality of life, and empowers individuals with POTS to regain their independence. Currently, with better access to wearable data and specialized protocols, movement is no longer just a challenge—it is the medicine that helps you stand tall again.

GnarlyTree | UNDERSTANDING POTS
What is POTS? | A Simple Guide to Postural Orthostatic Tachycardia Syndrome
A straightforward introduction to POTS, its symptoms, diagnostic criteria, and supportive management options.
Have you found that supplementing for any nutritional deficiency helped your symptoms?

