Table of Contents
Hypovolemic POTS is a distinct subtype of POTS and falls within the broader group of autonomic nervous system disorders known as dysautonomia. This form of POTS is primarily characterized by a reduced blood volume (hypovolemia), which affects the body’s ability to maintain proper blood flow when upright. Currently, research has increasingly focused on functional hypovolemia—where a patient may have a normal total fluid count, but the blood is “leaking” into surrounding tissues or pooling in the extremities due to poor vascular tone.
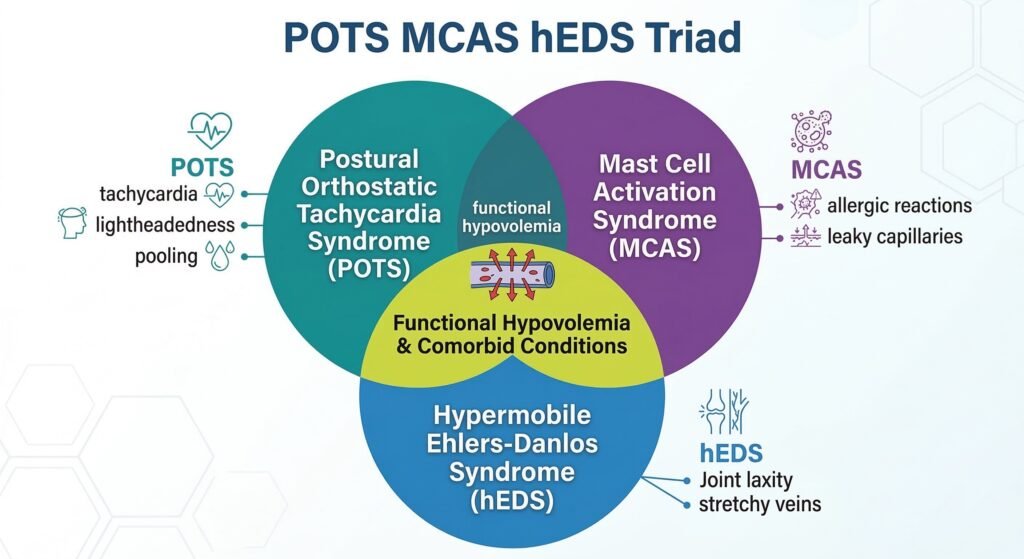
This lack of circulating volume leads to a cascade of symptoms that can severely affect daily functioning. Understanding hypovolemic POTS is crucial because it often exists as part of a clinical triad involving Mast Cell Activation Syndrome (MCAS) and Hypermobile Ehlers-Danlos Syndrome (hEDS). In these cases, “stretchy” veins or inflammatory “leaky” capillaries prevent the body from keeping blood where it belongs—in the vessels and moving toward the brain.
In this post, we will explore the nature of hypovolemic POTS, its symptoms, causes (including the Renin-Aldosterone paradox), diagnostic criteria, and the latest treatment approaches centered on increasing both volume and vascular “squeeze.”
Defining Hypovolemic POTS
Beyond Dehydration: Understanding Functional Hypovolemia and the POTS Triad.
Hypovolemic POTS is characterized by a reduced circulating blood volume, which results in inadequate venous return to the heart when standing. This deficiency causes a “mismatch” between the blood available and the blood needed for the brain and organs. To compensate for this reduced perfusion, the heart pumps faster—tachycardia—in an attempt to keep oxygen flowing upward against gravity.
Common Symptoms of Hypovolemic POTS
- Rapid heart rate upon standing: The hallmark compensation for low volume.
- Profound Fatigue: Often described as a “heavy” or “drained” feeling that doesn’t improve with rest.
- Lightheadedness or dizziness: Especially when transitioning from sitting to standing.
- Nausea & GI distress: Blood is shunted away from the gut to protect the heart and brain.
- Neurocognitive Dysfunction (Brain Fog): A direct result of reduced cerebral blood flow.
- Exercise intolerance: Difficulty with upright activity, though horizontal exercise may be better tolerated.
- Cold extremities: Vasoconstriction in the hands and feet as the body tries to keep blood in the core.
- Palpitations & Shakiness: Often driven by a secondary surge of adrenaline (norepinephrine) as the body “panics” over the low volume.
- Low blood pressure: While not always present, it is more common in the hypovolemic subtype than in hyperadrenergic POTS.

Key Triggers & Worsening Factors
These symptoms often worsen with:
Dehydration & Morning Hours: Symptoms are typically most severe in the morning when blood volume is naturally at its lowest point of the day.
Heat exposure: Heat causes vasodilation (widening of blood vessels), which makes it even harder for low volume to reach the heart.
Post-Prandial Pooling: After meals, the body sends a large amount of blood to the digestive tract. For a hypovolemic patient, this “steals” too much blood from the general circulation, leading to a massive spike in symptoms after eating.
Causes and Risk Factors
While the exact trigger for hypovolemic POTS can vary, it is increasingly understood as a multi-system failure. Key contributing factors include:
- Low Plasma and Red Blood Cell Volume: Many patients have a literal deficit in circulating blood. Research shows that some patients may have up to 15-20% less blood volume than a healthy person of the same size, which directly reduces cardiac output.
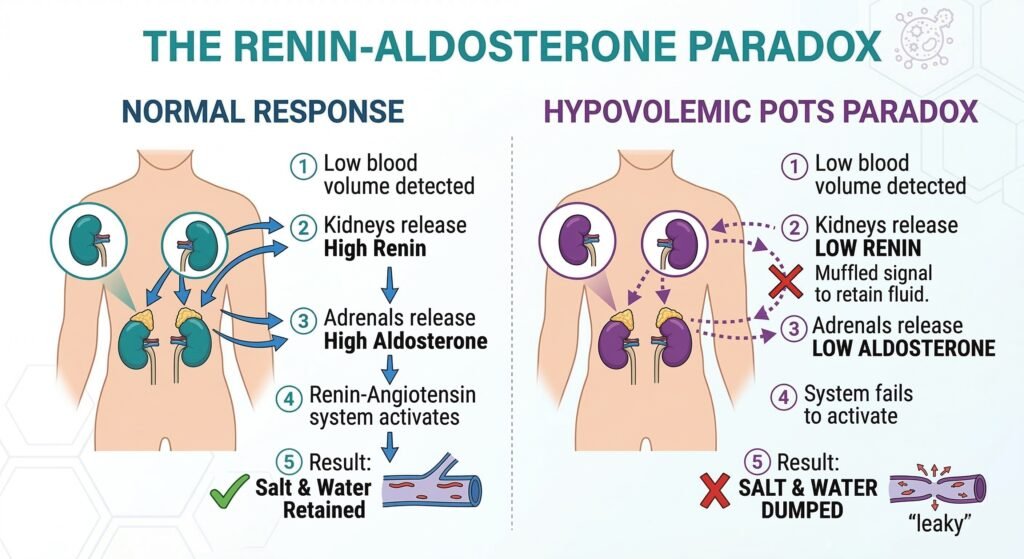
- The Renin-Aldosterone Paradox (RAAS Dysfunction): This is the “broken thermostat” of POTS. Normally, when blood volume is low, the body produces Renin and Aldosterone to retain salt and water. In many hypovolemic POTS patients, these hormone levels remain inappropriately low despite the dehydration, preventing the body from “holding onto” the fluids you drink.
- Post-Viral Onset & Autoimmunity: Viral infections (including COVID-19, EBV, and others) can trigger an immune response that mistakenly attacks the autonomic nervous system. By 2026, we’ve identified specific G-protein coupled receptor (GPCR) antibodies in some patients that may interfere with how blood vessels constrict, leading to “functional” volume loss.
- Capillary Leak (The MCAS Connection): Often triggered by inflammation, “leaky” capillaries allow the liquid part of your blood (plasma) to escape into surrounding tissues. This makes you feel dehydrated even if you are drinking gallons of water.
- Genetics and Connective Tissue Disorders: A strong correlation exists between hypovolemic POTS and Hypermobile Ehlers-Danlos Syndrome (hEDS). In these cases, “stretchy” blood vessels fail to provide the structural support needed to push blood back up to the heart.
- Chronic Dehydration: While not usually the primary cause, it acts as a severe “force multiplier” that makes underlying autonomic dysfunction much worse.
Diagnosing Hypovolemic POTS
Proper diagnosis is essential to distinguish hypovolemic POTS from other subtypes like Hyperadrenergic or Neuropathic POTS, as the treatment for “low volume” is very different from the treatment for “high adrenaline.”
Clinical Evaluation
A thorough review of symptoms and history is the first step. This includes assessing the impact of standing, diet, hydration status, and any “triggers” like previous viral illnesses, surgeries, or pregnancy. In 2026, clinicians also look closely for signs of comorbidities like joint hypermobility or mast cell activation.
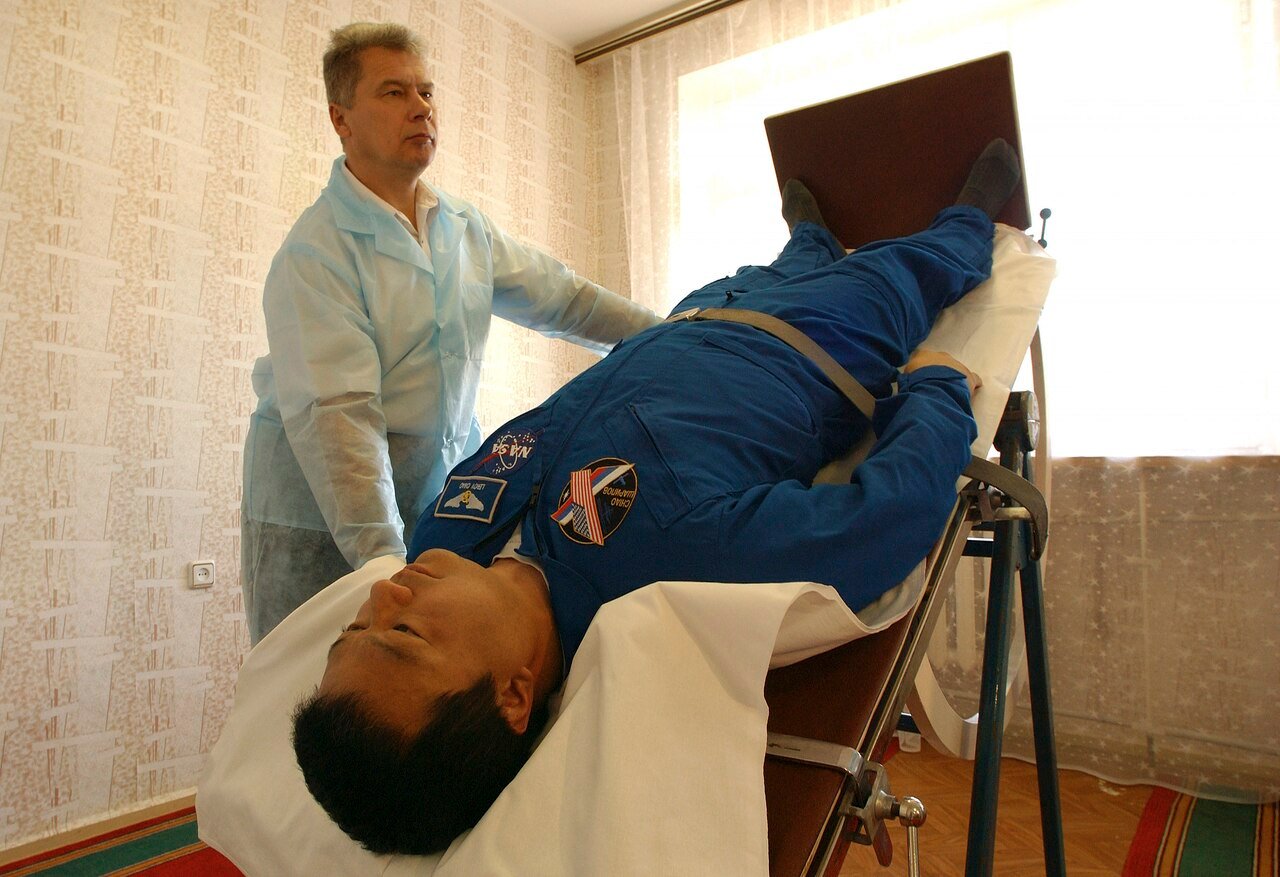
Tilt Table Testing (TTT)
The TTT remains a primary tool to evaluate heart rate and blood pressure response during changes in posture. In a classic hypovolemic POTS presentation, a significant heart rate increase (30+ bpm) occurs without a significant drop in blood pressure (which would instead indicate orthostatic hypotension).
Nuclear Blood Volume Analysis (BVA)
While previously rare, BVA-100 (Nuclear Medicine) testing has become the “Gold Standard” for confirming this specific subtype. By using a safe, radioactive tracer, doctors can measure the exact volume of plasma and red blood cells in your body. This allows for a definitive diagnosis: if your BVA shows a 10%–20% deficit, you are clinically hypovolemic.
The RAAS Profile (Hormonal Testing)
Assessment of the Renin-Angiotensin-Aldosterone System (RAAS) is vital. Doctors check for “low-renin, low-aldosterone” levels while the patient is upright. If these hormones don’t rise as they should when you stand, it confirms the body isn’t signaling the kidneys to hold onto fluid.
Wearable Biomarker Tracking
Many specialists now integrate data from clinical-grade wearables to monitor Heart Rate Variability (HRV) and “burden of tachycardia” over a 7-day period. This provides a “real-world” look at how volume fluctuates outside the clinic.

Treatment and Management of Hypovolemic POTS
Effective management for this subtype focuses on two primary goals: increasing total blood volume and improving vascular “squeeze” (tone) to prevent blood from pooling in the legs.
Lifestyle Modifications & “Volume Loading”
- Precision Hydration (2-3 Liters): It’s not just about water. In 2026, specialists emphasize Oral Rehydration Salts (ORS). Plain water can dilute existing electrolytes, triggering the kidneys to flush fluid out. Using high-quality electrolytes with a specific glucose-to-sodium ratio (the “sodium-glucose cotransport system”) pulls water directly into the bloodstream more effectively.
- High Salt Intake (5,000–10,000 mg): While 3,000 mg was the old standard, many hypovolemic patients now require 5,000 to 10,000 mg of sodium daily to overcome the “Renin-Aldosterone” deficit. Note: Always do this under medical supervision to monitor blood pressure.
- Advanced Compression: Research has shown that knee-high socks are often insufficient. Abdominal compression or waist-high garments (20-30 mmHg or 30-40 mmHg) are the gold standard because the largest volume of blood pools in the splanchnic (abdominal) bed and thighs.
- The Levine/Chop Protocol: Recumbent exercise remains the “medicine” for POTS. Rowing, swimming, and recumbent biking allow the heart to strengthen without the stress of gravity, eventually “remodeling” the heart to handle higher volumes.

Medications
- Fludrocortisone (Florinef): A mineralocorticoid that mimics aldosterone, telling your kidneys to “save” salt and water.
- Desmopressin (DDAVP): Often used for “rescue” or for patients who struggle with overnight volume loss, this hormone reduces urine production to keep fluid in the vessels.
- Midodrine & Mestinon: Midodrine acts as a vasoconstrictor to “squeeze” the veins. Mestinon (Pyridostigmine) is increasingly used in 2026 to improve the “break” (parasympathetic) signal of the nervous system and improve muscle tone.
- Ivabradine (Corlanor): Unlike traditional beta-blockers which can lower blood pressure (not ideal for hypovolemic patients), Ivabradine lowers the heart rate without affecting blood pressure, making it a favorite for this subtype.
Nutritional Support & Electrolyte Bioavailability
A nutrient-dense diet is essential, but the form of supplements matters.
Small, Frequent Meals: To avoid “post-prandial pooling,” eating 5-6 small meals rather than 3 large ones keeps blood from rushing to the gut all at once.
Magnesium Glycinate: Highly bioavailable and less likely to cause the “laxative effect” that can lead to further volume loss.
B-Vitamin Complex: Vital for mitochondrial health and energy production, which is often depleted by chronic “tachycardia fatigue.”

Living with Hypovolemic POTS and Dysautonomia
Living with hypovolemic POTS is a marathon, not a sprint. It requires a shift from “pushing through” to strategic energy management. The Neuro-Psychological Impact It is important to recognize that the “anxiety” or “jitteriness” many patients feel is often physiological, not psychological. When blood volume is low, the body compensates by releasing extra norepinephrine (adrenaline) to keep the heart pumping. This can trigger a “false” fight-or-flight response.
- Brain Fog & Mental Fatigue: This isn’t just “forgetfulness”—it is cerebral hypoperfusion (literally not enough blood reaching the brain).
- Supportive Therapies: While Cognitive Behavioral Therapy (CBT) can help manage the stress of chronic illness, many 2026 patients find more success with Heart Rate Variability (HRV) Pacing. By using wearables to monitor their “stress score,” patients can learn to rest before a crash happens.
- Trauma-Informed Care: Dealing with medical gaslighting is a common part of the POTS journey. Seeking providers who understand the “invisible” nature of this disability is crucial for mental well-being.
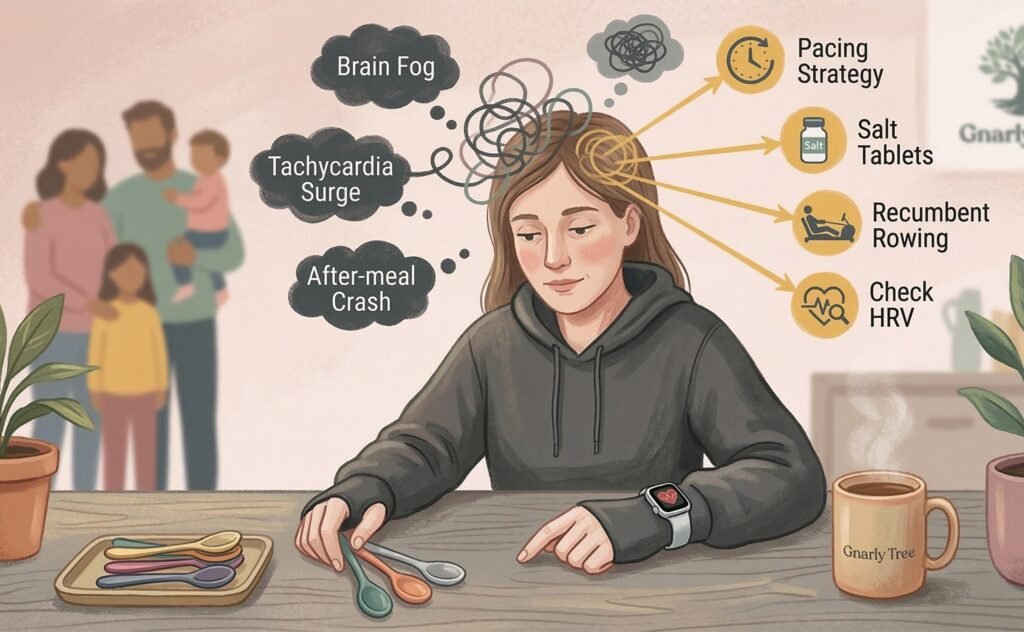
Strategic Pacing and “Spoon Theory”
Effective living requires radical acceptance of one’s physical limits. The “Spoon Theory” remains a vital tool for explaining energy conservation to friends and family, but modern management also includes:
- Pre-loading: Aggressively hydrating and salting before known stressors (like a shower or a doctor’s appointment).
- The 10-Minute Rule: If you feel a “dip” in energy, lay down with your legs elevated for 10 minutes to reset your venous return.
Community and Advocacy
You are not alone. The dysautonomia community has become a powerhouse of patient-led research.
Local Support Groups: Engaging in online forums or local meetups can provide the “hacks” that only fellow “POTSies” know—like which salt tablets taste the best or which compression leggings actually stay up.
Dysautonomia International: Still the gold standard for global advocacy and finding POTS-literate doctors.
Patient-Led Research Collaborative: A great resource for those interested in how post-viral research is shaping new POTS treatments.
GnarlyTree | NON-MEDICAL EQUIPMENT
Medical Alert for POTS | Bracelet, Wallet Card, Watchband Clip, Keychain Tag & More
A guide to medical alert options that help communicate POTS needs quickly during emergencies or unexpected symptom flares.
Frequently Asked Questions for Hypovolemic POTS
Is Hypovolemic POTS reversible? Currently, we view “remission” as a more accurate term than “cure.” While many patients experience significant symptom improvement through consistent “volume loading” and cardiac conditioning, the underlying physiological tendency toward low volume often requires long-term maintenance. For some, addressing a primary trigger (like a specific vitamin deficiency or an autoimmune marker) can lead to near-total resolution.
How is it different from simple dehydration? This is a critical distinction. Dehydration is a temporary state caused by not drinking enough. Hypovolemic POTS is a chronic regulatory failure. Even when a patient is drinking 3 liters of water, their body may “dump” that fluid rather than keeping it in the bloodstream due to the Renin-Aldosterone Paradox. You aren’t just “thirsty”; your body’s “tank” has a leak or a broken gauge.
Can I have more than one type of POTS? Yes, and many people do. This is often called “Mixed POTS.” You might have a low blood volume (Hypovolemic) while simultaneously experiencing a massive adrenaline surge when you stand (Hyperadrenergic). In these cases, doctors usually prioritize stabilizing the blood volume first, as the “low tank” is often what triggers the adrenaline surge in the first place.
Can I exercise with Hypovolemic POTS? Absolutely—in fact, it is a cornerstone of recovery—but it must be recumbent. Gravity is the enemy of a hypovolemic patient. By using a rowing machine, recumbent bike, or swimming, you can strengthen the heart and increase total blood volume without the dizziness and palpitations that come from standing.
Conclusion
Hypovolemic POTS is a challenging, invisible, yet highly manageable form of dysautonomia. It isn’t just a matter of “drinking more water”; it is a complex intersection of blood volume, hormonal signaling, and vascular tone. By 2026, the shift toward objective testing like Nuclear Blood Volume Analysis has made it easier than ever to get a personalized treatment plan that works.
With an accurate diagnosis and a commitment to strategic hydration, high-grade compression, and recumbent conditioning, many patients can regain their functionality and significantly improve their quality of life. If you suspect your “dizziness” is actually a volume issue, consult a dysautonomia specialist to explore your RAAS profile and volume status.

What is the most helpful non-medical aid you use?